Auto Added by WPeMatico

Insurance companies have imposed unwritten quotas limiting inpatient admissions, forcing doctors to make difficult judgement calls that could carry long-term health consequences for patients
by AZALEA AZUAR & SHAUQI WAHAB
CONCERNS over insurers influencing clinical decision-making in private hospitals have intensified after reports that doctors are facing pressure to prioritise outpatient care and manage admissions to meet insurer expectations.
In January, a doctor reportedly told an online portal that insurance companies have imposed unwritten quotas limiting inpatient admissions.
These pressures, relayed informally through hospitals, have forced doctors to make difficult judgement calls that could carry long-term health consequences for patients.
The pressure stems from a new initiative that allows policyholders to access outpatient treatment at private hospitals without prior payment guarantees.
Under this arrangement, doctors are encouraged to manage illnesses such as dengue, influenza and gastroenteritis as outpatients, even in cases where admission may be clinically necessary.
Hospitals, fearing removal from insurers’ panels, are said to relay these expectations to doctors through informal messages.
Doctors warn that such unwritten insurer quotas risk undermining professional judgement and shifting treatment decisions toward insurer-driven cost controls.
Compromising Patient Safety Erodes Trust
Private Medical Practitioners’ Association of Selangor and Kuala Lumpur (PMPASKL) president Dr Eugene Chooi said these developments have raised concerns that such policies may compromise clinical autonomy and patient safety.
He argued that financial targets should never override clinical decisions, even as insurance companies pursue cost containment.
“Clinical decisions must be guided by a patient’s condition, risk profile and need for monitoring, not by financial targets set by third parties.
“Managing conditions such as dengue, influenza or gastrointestinal illnesses as outpatients may be appropriate in selected cases, but forcing such decisions through insurer pressure increases the risk of delayed treatment, complications and avoidable harm,” he told The Malaysian Reserve (TMR).
Dr Chooi stressed that medicine relies on professional judgement and patient welfare, warning that cutting costs at the expense of care could lead to complications, re-admissions and loss of trust in the healthcare system.
“Saving money and delivering quality healthcare must go hand in hand; one cannot be achieved at the expense of the other,” he said.
He added that sustainable healthcare requires transparent, evidence-based frameworks that respect doctors’ judgement and focus on value-based care rather than rigid cost-cutting that risks patient safety.

Dr Chooi argues that financial targets set by 3rd parties should never override clinical decisions
Shifting Power Away from Clinicians
Universiti Malaya (UM) economist Dr Goh Lim Thye said if reports of tighter approvals and utilisation controls are accurate, private hospitals risk becoming administrative enforcers of insurer cost-containment strategies.
He said this dynamic could gradually shift power away from clinicians and towards insurer- driven rules, raising concerns about delays and compromised decision-making in borderline or time-sensitive cases.
When hospitals act as intermediaries to implement insurer approval requirements, they will no longer have pricing power. That power will slowly shift to the payers, meaning the insurance companies.
“This would shift influence away from clinical judgement toward administrative decision-making, with pricing power moving from providers to insurer-driven rules and approvals,” he said.
Goh warned that such a shift risks eroding clinical autonomy without necessarily addressing the root causes of rising healthcare costs.
The more critical policy question, he argued, is what is driving insurer pressure in the first place.
If cost escalation stems from overpricing, inconsistent billing or weak price discipline among certain providers, then intervention should occur at an institutional level through audits, benchmarking, renegotiation of contracts or exclusion of persistently high-cost hospitals.
On the increasingly common “outpatient-first” model, Goh said such approaches can reduce costs when they appropriately substitute inpatient care without increasing follow-up visits or complications.
However, problems arise when outpatient-only pathways fragment care or delay definitive treatment, leading to deterioration that ultimately requires hospitalisation.
In these cases, apparent insurer savings may simply be shifted downstream to patients through repeated visits, additional diagnostics, time costs and higher out-of-pocket spending, or even to public hospitals when conditions worsen.
Dr Goh cited a 2019 Universiti Kebangsaan Malaysia (UKM) study estimating the average direct cost of an outpatient episode at around RM141, compared to approximately RM2,527 per inpatient admission — nearly an 18-fold difference even before recent healthcare inflation.
While this gap explains why insurers focus heavily on inpatient admissions, he cautioned that targeting inpatient costs alone does not guarantee lower system-wide spending if care is delayed or fragmented.
When outpatient-only treatment contributes to complications that later require hospitalisation, risks are unevenly distributed.
Patients bear the health consequences and indirect costs of delay, doctors remain professionally accountable for outcomes and hospitals face reputational and operational fallout, while insurers may influence pathways without bearing proportional downstream risk.
“This raises concerns about under-treatment rather than overuse, particularly in time-sensitive or borderline cases,” he said.
Over time, strong insurer influence over approvals can also create the perception of a two-tier system, where insured patients face more administrative hurdles than self-paying patients who can proceed without payer controls.
A more sustainable solution, Goh said, lies in tackling price variation directly by comparing what the same procedures cost across comparable settings and addressing differences in overheads, procurement, billing practices or margins — rather than shaping treatment decisions through administrative rules.
Managed Care, Moral Hazard and Unequal Access
UKM Faculty of Medicine public health medical expert Prof Dr Sharifa Ezat Wan Puteh said some managed care organisations (MCOs) and insurance companies are accused of practising “moral hazard” by deliberately minimising hospital admissions to reduce healthcare costs and limit payouts.
Such practices include restricting access through limited provider networks, prior authorisation requirements and utilisation reviews.
Treatments and reimbursements are often capped based on pre-agreed budgets tied to premiums, with providers paid only within narrowly defined cost ranges.
“This usually overrides the doctor’s clinical judgement and may not be the best outcome for the patient,” she said.
As a result, Dr Sharifa Ezat warned that patients may face lower satisfaction and quality of care, longer waiting times to see doctors and additional out-of-pocket costs such as copayments. They may also be pushed towards self-care or cheaper alternative medications, which can lead to more severe illness or complications.
She added that insurer control over patient care has been common for many years, particularly among private providers and general practitioners.

Dr Sharifa Ezat notes that insurer control over patient care has been common for many years (pic: MEDIA MULIA)
In September 2025, the Malaysian Medical Association (MMA) reportedly criticised third-party administrators (TPAs) for enforcing generic-only medicine policies in private healthcare, saying such rules threaten doctors’ ethics, patient rights and proper care.
A CodeBlue survey in October 2025 found most of 855 private healthcare specialists reported patients facing insurance-related problems over the past year.
Meanwhile, another news report on Feb 25 last year said several private hospitals risk being removed from insurance panels after failing to meet high discount demands from insurers.
The Association of Private Hospitals Malaysia (APHM) has since advised policy- holders to check hospital panel status to avoid access issues or delays in care.
Dr Sharifa Ezat said patients must follow rules set by insurance companies — based on agreed premiums and coverage — or by a TPA under contracts with employers.
“In many cases, patients have to pay extra on their own either in form of copayment, co-insurance or full payment themselves that put clients at risk of catastrophic health expenditure or complications due to the delay,” she told TMR.
While some insurers promote preventive care, managed controls can still influence how patients seek treatment.
“This can lead to inequality in access and lower healthcare outcomes in general.
“The fee for the service method is associated with higher patient satisfaction, wider health providers access, but will increase overall healthcare cost,” she said.
Higher-income patients may benefit from broader coverage, while clinicians in private hospitals must often follow insurer rules unless patients can afford copayments, supplementary insurance or upgraded plans.
No Authority Over Clinical Decisions
While insurers may attempt to influence treatment through coverage rules or informal communication, Malaysian law places the responsibility for clinical decisions squarely on doctors and hospitals.
Constitutional lawyer GK Ganesan Kasinathan said informal communications — including messages sent through platforms such as WhatsApp — can become relevant if disputes arise over patient care.
Under Malaysian law, such messages may qualify as documentary evidence if they show attempts by insurers to influence treatment decisions or coverage expectations.
“WhatsApp messages count as ‘documents’ in Malaysian courts and can prove what an insurer told a doctor about coverage or treatment expectations,” he told TMR.
However, these communications do not override professional obligations. Doctors remain responsible for exercising independent clinical judgement and may face negligence claims if cost considerations override what a reasonably competent practitioner would have done.
Private hospitals also carry legal responsibilities. Malaysian courts have consistently held that hospitals owe patients a non-delegable duty of care, meaning they must ensure a safe and appropriate system of treatment even when specialists are engaged as independent contractors.
Ganesan said insurers or TPAs could also face legal action if denial, delay or conditional approval of coverage contributes to patient harm.
“Courts are likely to look at all three — doctor, hospital and insurer — and then apportion blame,” he said.
Lawyer Mahmud Abdul Jumaat said Malaysian law also draws a clear line between commercial pressure and clinical authority.
He said insurers are not medical practitioners and therefore cannot lawfully dictate treatment pathways.
Any limitation on care must be clearly stated in the written insurance policy and disclosed to patients.
“Undocumented or informal instructions are legally weak and may expose insurers or hospitals to regulatory scrutiny if they interfere with patient care,” he said.
Mahmud added that while hospitals may engage in legitimate cost-management practices such as negotiating package rates or requesting justification for admissions, legal risks arise when financial considerations begin to shape clinical judgement.
Doctors who resist insurer-driven treatment limitations are generally protected under Malaysian medical ethics and common law, which require practitioners to exercise independent professional judgement.
Where refusal results in termination of contracts, loss of privileges or income disruption, doctors may have recourse through contractual claims, civil litigation or regulatory complaints.
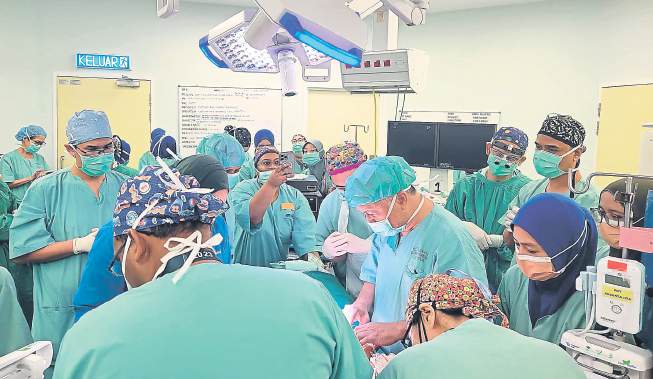
Sustainable healthcare requires transparent, evidence-based frameworks that respect doctors’ judgement and focus on value-based care (Source: Ministry of Health’s Facebook)
Clearer Insurance Frameworks
Angsana Health CEO and health systems specialist Dr Khor Swee Kheng said the insurance industry plays a crucial role in Malaysia’s health system but must better balance cost control with patient welfare.
Ideally, insurers will deliver preventive care, eliminate waste and abuse, and encourage evidence-based practice.
“The tendency of clinicians and patients may err towards increasingly more curative treatment, because of the moral hazard, defensive medicine, an abundance of caution or a desire for ‘instant cures’ without the difficulty of daily healthy habits,” he told TMR.
Dr Khor proposed a systematic claims framework backed by independent review for complex cases.
Regulatory efforts are also underway. In November 2025, the Health Ministry (MOH) and Bank Negara Malaysia (BNM) reactivated the Grievance Mechanism Committee (GMC) to improve collaboration, transparency and fairness in medical claims.
In December, BNM said insurers and takaful operators must settle claims fairly and promptly, though strict timelines remain undefined.
Opposition MPs have also called for stricter regulation after reports that a stage- four cancer patient’s claims remained unpaid for months, forcing tens of thousands of ring- git in out-of-pocket expenses.
Similar Cases Abroad
Malaysia is not alone in grappling with insurer influence over healthcare decisions. In the US, doctors and hospitals have long criticised insurer-driven treatment restrictions.
A Guardian investigation in May 2025 reported that UnitedHealth Group paid bonuses to nursing homes to reduce hospital transfers, which in some cases led to delayed treatment and harm.
In Australia, insurer British United Provident Association Ltd (Bupa) agreed to pay a proposed A$35 million (RM97.19 million) fine after admitting to wrongly denying valid claims over several years, according to the Financial Times.
Ultimately, experts said as Malaysia’s private healthcare system becomes increasingly intertwined with insurance-driven payment models, clearer rules governing insurer-provider relationships may be needed to ensure that treatment decisions remain guided first by clinical need rather than administrative targets.
When asked to comment on reports that doctors were concerned certain insurers were pushing hospitals to treat common illnesses on an outpatient basis, MCIS Life CCE and marketing officer Chitra Sridharan said that her company does not practise this.
“Medical decisions rest solely with healthcare professionals and we do not impose quotas or measures that influence clinical judgment or patient care pathways,” she told TMR .
Meanwhile, although Allianz General Insurance Co (M) Bhd declined to comment on the matter, it acknowledged that the issue continues to evolve due to rising health costs and the ageing population.
- This article first appeared in The Malaysian Reserve weekly print edition
The post Are doctors in charge of your treatment — or insurers? appeared first on The Malaysian Reserve.










